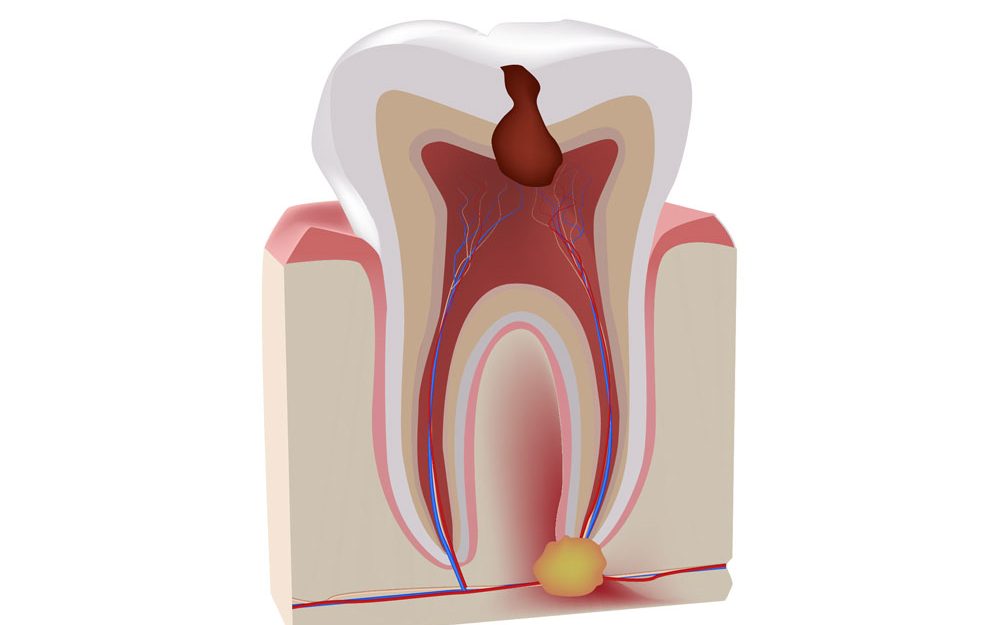
We all know that brushing twice daily is crucial in maintaining good oral hygiene, preventing oral diseases, and keeping our body healthy. Brushing and flossing correctly helps to remove the plaque build-up and also eliminates disease-causing bacteria. This prevents gum diseases and lowers the chances of getting dental decay and all the unpleasant consequences which comes with it. It also helps with proper digestion and reduces the chances of respiratory illnesses.
However, improper and faulty brushing habits can irritate and traumatise the gums. Therefore, it is crucial to learn the correct way of how to brush your teeth.
Before we jump on how to brush your teeth correctly, we must ensure that we have all the tools needed. To ensure that you are brushing correctly without hurting your gums, the first step is to procure a good quality toothbrush. Using a lousy quality and hard-bristled toothbrush is a sure-shot way of damaging your teeth and hurting your gums. Look for a toothbrush with softer bristles but not so soft that it doesn’t do its job.
Next, you want to get a good quality toothpaste that contains fluoride. Fluoride helps strengthen the tooth structure and reduces the chances of dental decay. Remember to replace your toothbrush every 3 months. If your toothbrush becomes frayed and warped, it loses its efficacy and also hurts the gums. You can also use an electric toothbrush. We will explain the mechanics of both in this blog.
How to brush your teeth correctly with a standard toothbrush?
After you have procured all the necessary tools for a perfect morning dental routine, it is now time to up your brushing game. It is vital to cover all the teeth surfaces, clean your gums and the tongue. A proper technique will help you achieve this by reaching all the corners of your teeth without damaging your gums.
STEP 1 – Wet your toothbrush with water and put a pea-sized amount of a fluoridated toothpaste on the toothbrush’s head.
STEP 2 – Put the brush in your mouth at a 45-degree angle to the gums. Use a gentle upwards stroke against the gum line to brush your upper and lower front teeth. These strokes should be gentle, short, and upward for lower teeth and downward for the upper front teeth. This helps you get rid of all the plaque and trapped food debris in your gum line, and at the same time, massages the gums.
STEP 3 – Use the same motion to brush the outer and top (chewing surfaces) of your upper and lower back teeth. This covers the exterior and top surfaces of all teeth in the mouth.
STEP 4 – Tilt the toothbrush upside down to reach the inner surface of the lower teeth. Brush the inner surface of all the lower teeth in a similar manner maintaining a 45-degree angle. Then flip the toothbrush to clean the inner surfaces of your upper teeth. Since the inner tooth surfaces are not visible, it can be very easy and often tempting to skip them. This slight ignorance is actually what causes plaque build-up and leads to gum diseases.
STEP 5 – Brush your tongue to remove all the build-up and bacteria. This will ensure fresher breath and healthy oral health. Rinse, and you are done!
How long should you brush?
Ideally, you should brush for at least 3 minutes. You can set a timer to ensure that you are giving your mouth the time it deserves. Overbrushing and using a hard-bristled toothbrush can damage the teeth as well as the gums. It can cause abrasion of teeth, lead to teeth sensitivity and cause gum recession.
How to brush your teeth with an electric toothbrush
STEP 1 – Wet the toothbrush head and use a pea-sized amount of toothpaste.
STEP 2 – Turn on the toothbrush and follow the same procedure as described above to brush the outer and top surfaces of your upper and lower teeth.
STEP 3 – Tilt the toothbrush to access the inner surfaces, just as described above. Ensure that you apply light pressure and move gently from one tooth to the other, involving all your teeth.
STEP 4 – Clean your tongue and rinse for fresher breath.
It is essential to learn the correct way of brushing to ensure that you have a clean mouth. Improper brushing will cause plaque build-up and lead to dental cavities and gum diseases. Many of us use the wrong technique to brush our teeth, and instead of protecting them, we end up harming them. However, now you know the best and the correct way to brush your teeth without destroying your gums. Use this technique to ensure that you always keep smiling and your pearly whites remain strong and disease-free.